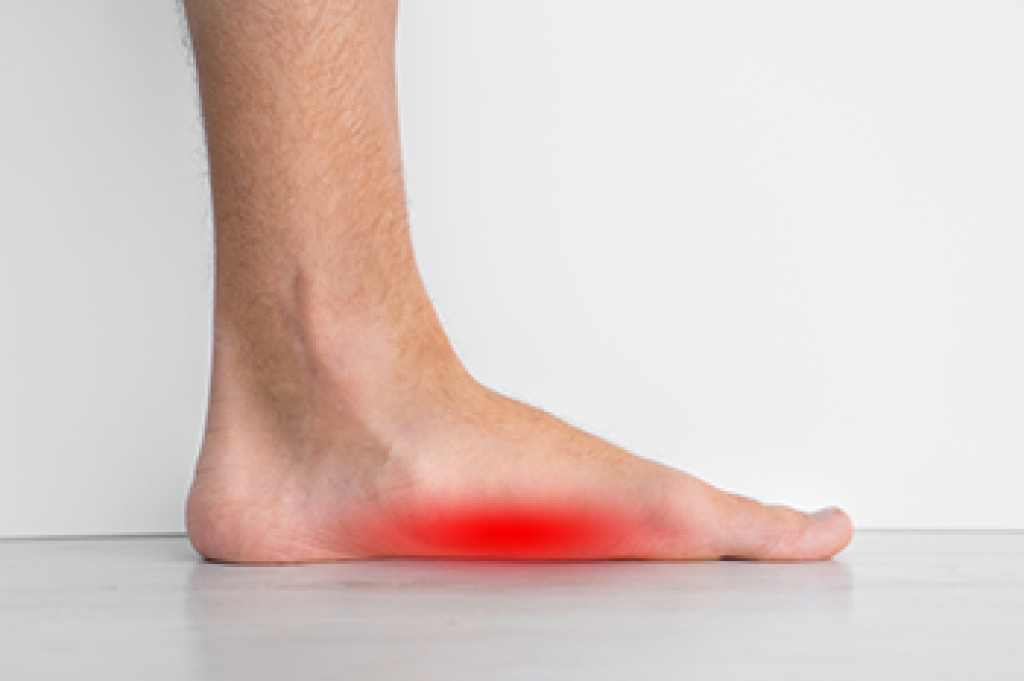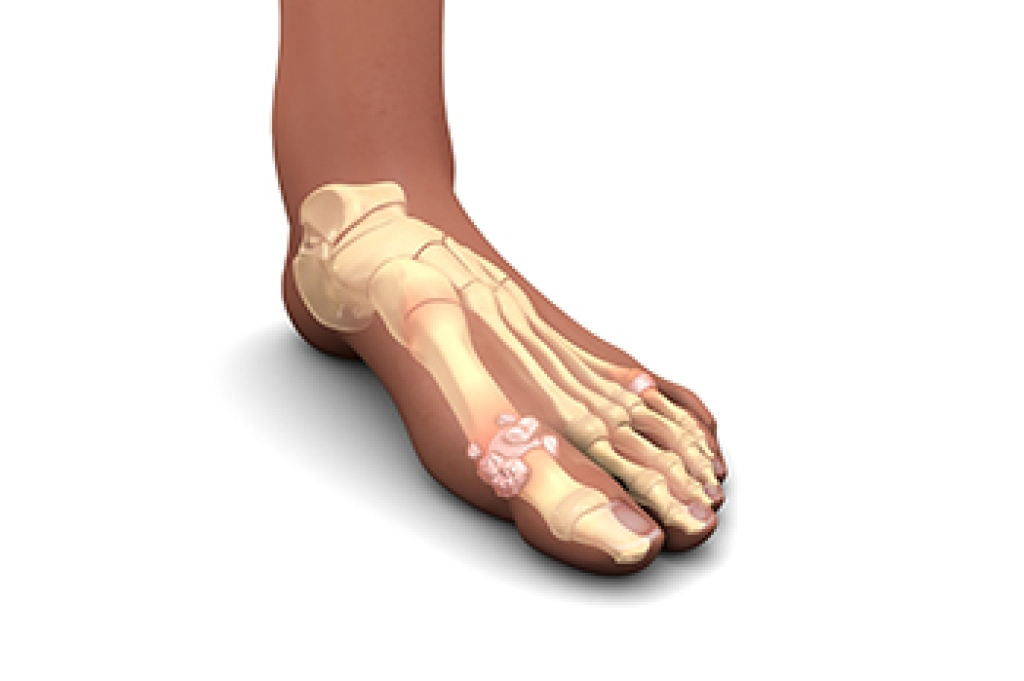
Gout is a form of inflammatory arthritis that develops when uric acid crystals build up in a joint, most often with severe pain in the big toe. The condition usually appears suddenly, often at night, with intense pain, redness, warmth, and swelling. Some people describe the pain as sharp and throbbing, making even light pressure uncomfortable. Risk factors include older age, diets high in red meat or sugary drinks, certain medications, and excess body weight. Gout happens when the body either produces too much uric acid or cannot remove it effectively. Flare-ups may come and go, but without proper care, they can become more frequent. A podiatrist can diagnose gout, confirm it with testing, and provide treatments that reduce pain and prevent joint damage. Gout can be very painful and may cause difficulty in completing daily tasks. If you have symptoms of gout, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this painful condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Leonard Talarico, DPM from Georgia. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Pooler, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.